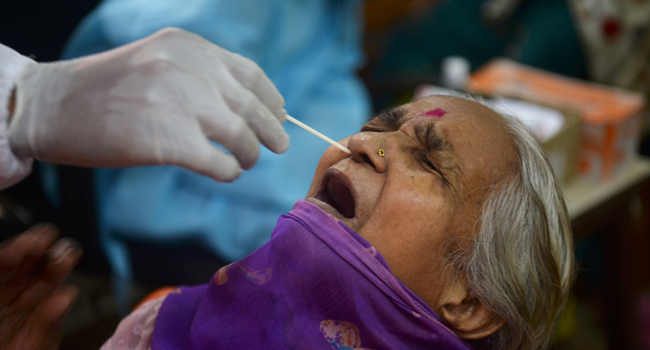
India’s official coronavirus death toll soared past 50,000 on Monday as the pandemic rages through smaller cities and rural areas where health care is feeble and stigmatisation rife.
Many experts say the real numbers may be far higher due to low testing rates and because deaths are often not properly recorded in the vast and impoverished nation of 1.3 billion people.
India last week overtook Britain with the world’s fourth-highest number of fatalities, behind the United States, Brazil and Mexico, and as of Monday had recorded 50,921 deaths, according to the health ministry.
With some of the world’s biggest megacities and slums, India is already the third-most infected nation behind the US and Brazil with 2.65 million infections.
Despite the rising death toll, the health ministry said on Sunday that India’s virus mortality rate of 1.92 percent was “one of the lowest globally”.
“Successful implementation of testing aggressively, tracking comprehensively and treating efficiently through a plethora of measures have contributed to the existing high level of recoveries,” the ministry said.
According to tracking website Worldometer, the United States, with 170,000 deaths, has a death rate of 3.11 percent while Brazil, with almost 110,000 fatalities, sees 3.22 percent of those who test positive die.
According to the Indian health ministry, the US “crossed 50,000 deaths in 23 days, Brazil in 95 days and Mexico in 141 days. India took 156 days to reach this national figure.”
Possible reasons that have been suggested include India’s relatively young population, its climate and greater exposure to pathogens that cause tuberculosis than elsewhere.
But experts say India’s testing rates per million inhabitants are far lower than other countries, and that too few deaths are properly recorded — even in normal times.
“(A) couple of studies have indicated that… only one in four deaths is certified and a cause of death is established,” Lalit Kant, former head of epidemiology and communicable diseases at the Indian Council of Medical Research, told AFP.
In addition, many of the tests being done — up to 30 percent nationally — are the less reliable rapid antigen tests where “false negatives” can be reported in up to half of cases, according to media reports.
Lockdown misery
Prime Minister Narendra Modi’s government imposed in March one of the world’s strictest lockdowns.
It dealt a heavy blow to Asia’s third-biggest economy and caused misery for the country’s poor, with tens of millions of migrant workers left jobless almost overnight.

Vast numbers trudged back penniless to their home villages from cities including New Delhi, Mumbai and Ahmedabad, many of them on foot. Some died on the way.
The lockdown has since been steadily eased but many sectors complain that they are severely short of workers.
State and local governments across the country have meanwhile reimposed lockdown measures as the virus has spread to smaller cities and rural areas, where around 70 percent of Indians live.
In many rural regions however, anecdotal evidence suggests that measures to stop the spread such as masks and distancing are widely ignored.
In addition, a lack of public awareness has contributed to those with the virus being ostracised, making people more reluctant to get tested.
Health care facilities outside the major cities are also severely stretched.
“In smaller cities and towns and rural areas tests of COVID-19 may not be available,” Lalit said.
“Patients with COVID-like symptoms are often turned away from heath care facilities, some may die without a test being done.”
AFP




